The difference between midwifery and obstetric models
This blog is a response to GP Obstetrician Dr. Taylor’s March 13th

on the Geraldton Guardian article, Mum Leads Midwife Push. I was honoured to be featured in the article where I discussed the necessity of access to a midwife-led care model for women in Geraldton and all of WA for that matter. Since the Guardian was unable to include our full interview, I believe Dr. Taylor misinterpreted my words (the fault of the short article, not his) and was therefore unable to hear the deeper and very important message that I, and many other women, have been raising our voices to say.
So let’s begin here:
There seems to be some confusion over just what that phrase, continuity of midwifery care, means.
Dr. Taylor stressed that “true continuity of care” already exists in Geraldton and we should not lose sight of the “brilliant service” already in place. If Dr. Taylor is reading this, please know that I firmly agree with the latter part of your statement but take issue with the former.
We do indeed have wonderful obstetric care in Geraldton and a strong model in place, and for that I am grateful. I’ve even twice been a consumer of those services; however, the services did not suit me as an individual.
For some women, this model is perfect and fits all their needs and desires. For myself and other women I know of, however, it was not thorough enough to be fully supportive and satisfactory to our birth experiences.
This is because the current model fails to include midwifery continuity of care which, as you will see in this blog, is quite different from the way GPs define continuity of care.
If we can collaborate to fill the gaps, then we can truly have a thriving and healthy community of empowered parents with a voice—and a choice—about where and with whom they give birth.
As both a birth doula and Hypnobirthing Australia ™ Practitioner, I look forward to working with Dr. Taylor in the future, helping women’s births become their own.
So without further ado, let’s dive right in!
What exactly is Midwifery Continuity of Care Model?
Midwifery Continuity of care model involves a small group of public hospital midwives who work together and even collaborate with GP doctors, if need be, to provide antenatal, labour and birth services to women.
Over the course of her pregnancy, a woman gets to know her midwife very well. Likewise, the midwife gets to know the woman very well and on all levels: physically, emotionally, mentally, and spiritually. A deep trust and friendship is formed. This kind of relationship supports a peaceful and safe birthing experience and allows for highly-personalized care.
The woman’s designated midwife is on-call for the birth, so the woman knows ahead of time exactly who will be with her in labour. This model also include up to six weeks of postnatal care, most of it taking place in the family’s own home.
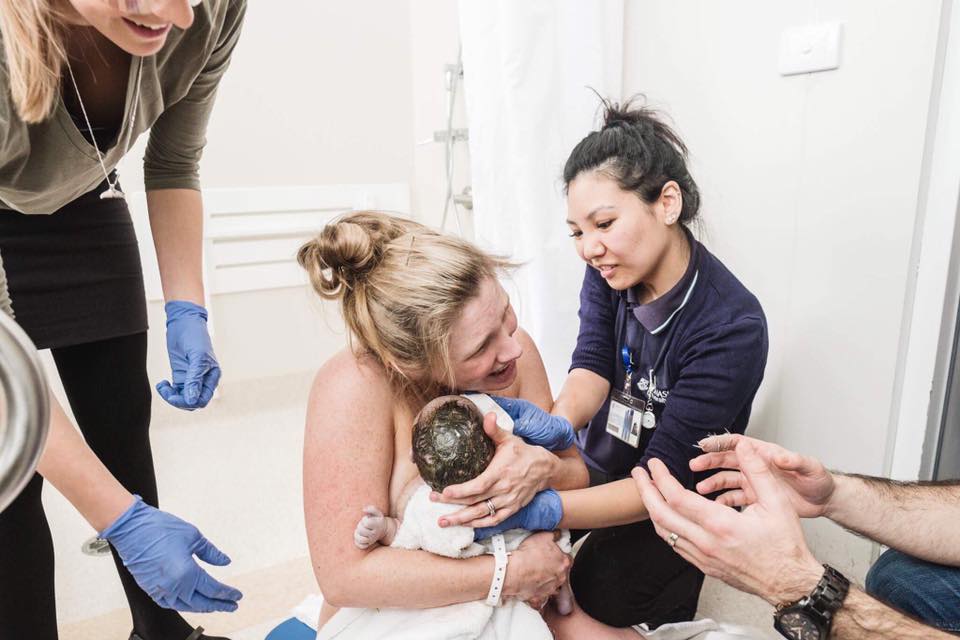
What else is great about Continuity of Midwifery Care?
Midwifery continuity of care models are associated with lower intervention rates. This includes caesarean section, instrumental deliveries (vacuum and forceps), and episiotomies (a cutting to make the vaginal opening wider).
According to both a Cochrane and a Lancet study, women are, overall, more satisfied with this model and the care is more cost effective.
Is the goal to eventually get rid of GP and Obstetric Care Models?
No way! I want ALL options easily accessible to women and then I want to let women choose!
Some women only want obstetric care and some even require it due to special circumstances. Other women want midwifery led care with very few interventions.
Every woman is uniquely different and deserves the right to birth in the way that feels is best for her and her baby.
Geraldton has a great obstetric model, but without offering a Midwifery Group Practice model of care then women don’t really have a choice.
Dr. Taylor said, and I’m sure many GPs would agree, that they “support a woman having a choice”. That’s nice. It’s a good place to start.
But, it’s not enough without advocating for the development of models that actually give us—women—a choice.
It’s time to invest in developing a Continuity of Midwifery Care model because less than 10% of women across Australia have access to that type of care!
Does Midwifery-Led Care threaten GP/Obstetrics?
I sure don’t think so.
I believe developing a Midwifery Group Practice model of care that works in collaboration with Geraldton’s obstetric model would both enhance and invigorate our community.
Besides, the main thing to worry about is not whether midwives threaten GPs or GPs threaten midwives, but truly—what is best for the mother?
Even WHO recommends that women have continuity of midwifery care according to their most recent guideline release, see Recommendation 4.3.1.4
Ok, but Dr. Taylor said continuity of care already exists! Is a Midwifery continuity of care model just being redundant?
In Dr. Taylors definition, true continuity of care meant delivering (see note below) a woman’s baby and later her grandbaby. It meant caring for uncles and siblings and grandparents. While this type of care is very beneficial and important, it is the extent of what a doctor can do and is not representative of midwifery led care.
Obstetricians are a necessary part of the birth team but they cannot be—with woman, the literally meaning of midwife— as a midwife can. Midwives are the people to support a woman in labour and it’s their expertise in physiological births which account for their better birth outcomes.
In the current obstetric model of care, a woman has access to meet with midwives maybe twice during her pregnancy, and at the time of birth her midwife is often someone she’s never met before! That’s not continuity of care.
Midwife models of care go beyond the normal 15-minute GP or OB appointment and take a full hour (or more!), multiple times throughout pregnancy. During this time the midwife considers every aspect of the mother’s needs: emotionally, spiritually, physically, mentally and socially. It is quite holistic.
(Please note caregivers are not there to “deliver babies”. This isn’t a Pizza Hut people. Pizzas are delivered. Babies are received. Only a mother can birth her child. Caregivers are, however, often in the best position to the baby if need be! Okay okay, language surrounding birth is really a whole other blog so I’ll get off my soap box!)
In Summary
Not only is there a strong need for Midwifery Continuity of Care models in Geraldton, but there is also a strong desire for it from the people who matter most in this issue—women.
A midwifery model can work side by side within the current obstetric models, is recommend by WHO, and can enhance our community by empowering birthing mothers.
I’m raising my voice for women and mothers.
Are we grateful for the stellar GP Ob services provided to us here in Geraldton? Yes.
But does our gratitude negate our right for more choice and less intervention? Certainly not.
I’m not here to fight or to tear down. I’m here to enlighten and enlist women, midwives, GPs, OBs, doulas, partners, and everyone on a birth team to create something new, something better, something necessary.
For further reading, The National Maternity Plan elaborates rather nicely on the principles of maternity care here.
Bio
My name is Melissa Ayling and I am a certified Hypnobirthing Australia™ practitioner, birth doula, and mother-blessing facilitator. I am extremely passionate about women being acknowledged during such a transformational and significant life event. I am based in Geraldton, Western Australia and you can learn more HERE about how I help women become experts in their own pregnancy and birth through independent childbirth classes like Hypnobirthing Australia™.